ADHD and Hormones in Women: How Estrogen Affects Symptoms
By Kristen McClure, MSW, LCSW | Neurodivergent-affirming therapy for women
You have been managing your ADHD — maybe for years, maybe your whole life. Then something shifts.
Your symptoms feel worse for a week every month. Or you reach your late thirties or forties and everything that used to work stops working. Or you have a baby and suddenly you cannot function the way you did before.
And nobody connects the dots.
Not your prescriber. Not your OB. Not the therapist you saw years ago.
This is one of the most common and most underdiscussed experiences for women with ADHD.
Hormones do not cause ADHD. But they can affect how ADHD shows up.
Estrogen, in particular, has a direct relationship with the dopamine systems that are already more vulnerable in ADHD. This means every major hormonal transition in a woman’s life — the menstrual cycle, postpartum, perimenopause, and menopause — can change how the ADHD brain functions.
Sometimes the change is dramatic.
If your ADHD symptoms feel inconsistent, unpredictable, or worse at a particular life stage, you are not imagining it. There is a biological explanation. There are also things you can do about it.
The Estrogen-Dopamine Connection
To understand why hormones matter for ADHD, it helps to understand one key relationship:
Estrogen supports dopamine function in the brain.
Dopamine plays a major role in attention, motivation, working memory, impulse control, reward, and emotional regulation. ADHD brains have differences in dopamine signaling, including how dopamine is produced, released, and reabsorbed.
Estrogen influences this system in several ways. It appears to support dopamine production, increase dopamine receptor sensitivity, and slow dopamine reabsorption. In simple terms, estrogen may help dopamine stay active longer.
When estrogen is higher, many ADHD women report that their brains feel sharper. Focus may improve. Emotional regulation may feel steadier. Tasks may feel easier to start and finish.
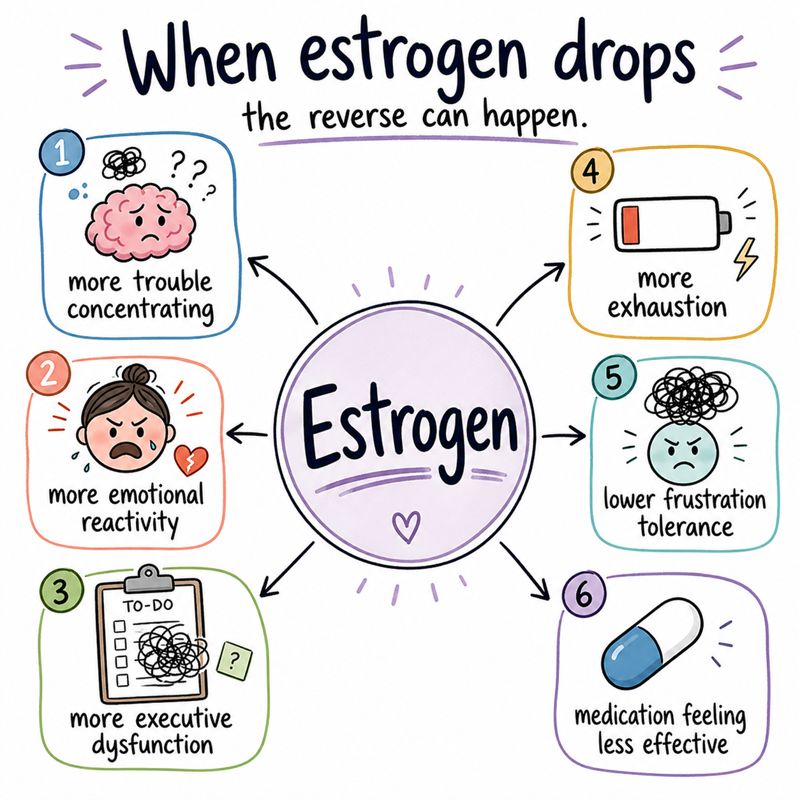
When estrogen drops, the reverse can happen.
- You may notice:
This is not a personality issue. It is not a lack of trying. It is a neurochemical shift happening in real time.
The research is still developing. ADHD research has historically focused more on boys and men, and the specific estrogen-dopamine connection in ADHD women is still not fully mapped.
But the clinical picture is clear. Many ADHD women experience symptom changes across hormonal shifts, and emerging science supports what many women have been describing for years.
Hormonal changes can hit ADHD brains harder.
ADHD and the Menstrual Cycle
For women with ADHD in their reproductive years, the menstrual cycle can create a predictable pattern of ADHD symptom changes.
Estrogen rises in the first half of the cycle, called the follicular phase. It peaks around ovulation. Then estrogen drops in the second half of the cycle, called the luteal phase, while progesterone becomes more dominant.
For many ADHD women, the follicular phase feels more functional.
Then, in the week or two before menstruation, ADHD symptoms may intensify.
You may notice:
This is sometimes described as premenstrual ADHD worsening. It is different from PMS, although the two can overlap.
The key difference is that for ADHD women, what worsens is not only mood. Core cognitive functioning can worsen too.
If you have ever felt like a completely different person in the week before your period, this may be part of the reason.
Tracking your cycle alongside your ADHD symptoms can be very useful. It does not eliminate the pattern, but it helps you see it clearly.
It can help you:
Your hardest week is not proof that you are failing. It may be a predictable pattern that needs support.
Learn more about ADHD and your period here
ADHD and PMDD
Premenstrual Dysphoric Disorder, or PMDD, is a severe form of premenstrual syndrome. It causes significant emotional and physical symptoms during the luteal phase. These symptoms usually improve after menstruation begins.
PMDD affects roughly 3–8% of women in the general population.
Among women with ADHD, the rate appears to be much higher. Some estimates suggest that women with ADHD may be up to three times more likely to meet criteria for PMDD.
The overlap makes clinical sense.
Both ADHD and PMDD involve dopamine and serotonin systems. Both can involve emotional dysregulation. When the luteal phase brings a drop in estrogen, it can affect a nervous system that is already more sensitive to changes in dopamine.
PMDD is not bad PMS.
It can include:
- severe depression
- rage
- anxiety
- dissociation
- suicidal thoughts
- intense rejection sensitivity
- major impairment for one to two weeks each month
When ADHD and PMDD occur together, the combination can be genuinely disabling.
PMDD is underdiagnosed. The overlap between ADHD and PMDD is also underrecognized.
If you suspect you may have both, that is important information to bring to your care team.
Treatment for PMDD may include:
- SSRIs, taken daily or during the luteal phase
- hormonal treatment to stabilize estrogen changes
- ADHD medication adjustments
- symptom tracking
- sleep and stress support
- careful planning around the luteal phase
You deserve treatment that addresses both ADHD and PMDD, not one while ignoring the other.
For a deeper look at the ADHD-PMDD overlap, including tracking tools and treatment options, see the full page on ADHD and PMDD.
ADHD in Perimenopause and Menopause
Perimenopause is the years-long transition before menopause. It often begins in the forties, though it can start earlier. During this time, estrogen becomes more erratic before eventually declining.
Perimenopause is one of the most common times for women to receive a first ADHD diagnosis.
This does not mean they suddenly developed ADHD.
It often means the estrogen decline removed a neurochemical support that had been helping them compensate for ADHD symptoms for years.
Many women had systems that worked. They masked. They overprepared. They relied on anxiety, structure, routines, or urgency to get through life.
Then perimenopause starts, and those strategies no longer work the same way.
Women may notice:
- worse focus
- unreliable memory
- more emotional reactivity
- stronger overwhelm
- more fatigue
- worse sleep
- reduced stress tolerance
- executive function that feels suddenly much harder
Because these symptoms also overlap with general perimenopause symptoms, they are often dismissed as normal menopause, stress, or aging.
But for ADHD women, perimenopause can make ADHD much harder to manage.
Menopause is defined as twelve consecutive months without a period. After menopause, estrogen stabilizes at a lower baseline.
For some women, ADHD symptoms stabilize after this point. For others, the lower estrogen baseline means ADHD remains harder to manage than it was earlier in adulthood.
Treatment may need to be adjusted.
The research on hormone replacement therapy, or HRT, and ADHD is limited but promising. Some women report better ADHD functioning with HRT. This makes sense given estrogen’s role in dopamine function, but it is still an emerging area.
HRT is a medical decision that needs careful discussion with a prescriber who understands your health history, risk factors, and symptoms.
If you are in perimenopause and struggling, and you have ADHD, you are not losing your mind. You are experiencing a real neurobiological change. For more detail on this transition, including what to track and how to advocate with your care team, see the full page on ADHD and Perimenopause.
ADHD Postpartum
The postpartum period is another major hormonal transition. It can be especially difficult for women with ADHD.
After delivery, estrogen and progesterone drop sharply. This is one of the steepest hormonal declines in human physiology.
For ADHD women, this drop happens during a period of:
- sleep deprivation
- physical recovery
- major life disruption
- constant task switching
- increased emotional demand
- reduced personal time
- high responsibility
This can create a serious strain on the ADHD brain.
Women with ADHD have higher rates of postpartum depression and postpartum anxiety than women without ADHD. This makes sense when you consider the hormonal, neurological, and environmental load.
Postpartum mood difficulties in ADHD women may require treatment that accounts for ADHD too.
That may include:
- sleep protection when possible
- medication planning
- executive function support
- help with routines
- realistic expectations
- support from partners, family, or professionals
- monitoring for postpartum depression and anxiety
The postpartum period is also when many women stop or pause ADHD medication because of breastfeeding concerns.
This decision deserves careful medical guidance. The risks of untreated ADHD in the postpartum period are real. These may include severe anxiety, depression, difficulty maintaining safety routines, difficulty with sleep, and difficulty bonding.
Medication decisions should weigh both the risks of medication exposure and the risks of untreated ADHD.
If you are pregnant, recently postpartum, or planning a pregnancy, having an explicit conversation with your care team about ADHD management through this transition is important. You don't have to white-knuckle it. For a detailed look at this period, see the full page on ADHD and Postpartum Depression.
What This Means for Treatment
The hormonal dimension of ADHD in women has practical implications for treatment.
Medication may need to be adjusted across the cycle
Some women work with prescribers to adjust stimulant medication during the luteal phase, when ADHD symptoms are more severe.
This is not standard for everyone. It requires careful monitoring. But it reflects an important reality:
A fixed ADHD medication dose may not feel the same at every hormonal phase.
Hormonal treatment may be part of the picture
For PMDD, hormonal approaches that stabilize estrogen changes may reduce monthly cognitive and emotional disruption.
For perimenopause, HRT may improve ADHD functioning for some women, though the ADHD-specific research is still developing.
Non-medication support matters
Medication is only one part of ADHD treatment.
During postpartum, perimenopause, or the luteal phase, other supports may become even more important.
These may include:
- simpler routines
- reduced demands
- external reminders
- support with meals and household tasks
- fewer unnecessary decisions
- more recovery time
- clear communication with family or partners
Cycle tracking is useful clinical information
You may want to track:

Tracking your menstrual cycle and ADHD symptoms can help you see patterns.
This information can help you make better decisions about scheduling, workload, medication conversations, and support.
Providers need to understand both ADHD and hormonal health
Finding providers who understand both ADHD and women’s hormonal health is harder than it should be.
You may need to be the person connecting the dots.
That is not fair. But knowing what to ask for makes advocacy easier.
How the Empowerment Model Addresses Hormonal Transitions
The hormonal dimension of ADHD is exactly the kind of experience the Empowerment Model is designed to help with.
It requires all five pillars working together.
Self-Awareness
Self-awareness means learning your own hormonal pattern.
This is not only knowing that hormones can affect ADHD. It means noticing how your specific brain responds across your cycle and across life stages.
You may begin to see that your hardest weeks have a pattern. That information changes how you plan, how you communicate, and how you understand yourself.
Self-Compassion
Hormonal ADHD worsening is easy to internalize as failure.
The week before your period, postpartum, or during perimenopause, you may tell yourself you are lazy, broken, inconsistent, or unreliable.
Self-compassion means pausing that self-blame long enough to look at what is happening.
Your brain may be managing a real neurochemical shift. Blaming yourself will not solve it. Support is more useful.
Self-Accommodation
Self-accommodation means adjusting your workload, commitments, and expectations to match your actual capacity.
This may mean:
- avoiding high-demand work during the luteal phase when possible
- reducing social commitments before your period
- planning more support postpartum
- simplifying routines during perimenopause
- building recovery time into your schedule
- asking for help before you hit a crisis point
Self-accommodation is not giving up. It is planning based on accurate information.
Self-Advocacy
Self-advocacy means talking directly with your providers about ADHD and hormones.
This may include your psychiatrist, primary care provider, OB, gynecologist, therapist, or ADHD coach.
You might ask:
- Could my ADHD symptoms be changing because of hormonal shifts?
- Could PMDD be part of this pattern?
- Should we track medication effectiveness across my cycle?
- Are there treatment options for luteal phase worsening?
- Could perimenopause be affecting my ADHD?
- Should we discuss HRT or other hormonal supports?
- How should I plan for ADHD treatment during pregnancy or postpartum?
Self-advocacy also means pushing back when your symptoms are dismissed as “just hormones” without treatment or support.
Self-Care
Self-care in this context means protecting the basics that support dopamine and nervous system functioning.
- This includes:
- sleep when possible
- food and hydration
- movement
- reduced overload
- sensory support
- recovery time
- lowering demands during more vulnerable phases
This kind of self-care is not decorative. It is part of ADHD support.
Frequently Asked Questions
For many women, yes.
Estrogen supports dopamine function, and ADHD involves differences in dopamine signaling. When estrogen drops before menstruation, postpartum, or during perimenopause, ADHD symptoms may intensify.
This does not always mean your ADHD is permanently worse. It means your symptoms may be responsive to your hormonal environment.
Perimenopause is a time of significant estrogen fluctuation and decline, which directly affects the dopamine systems involved in ADHD. Many women with undiagnosed ADHD first seek help during perimenopause because compensatory strategies that worked for years suddenly stop working. If you are in your forties and experiencing a significant decline in focus, memory, emotional regulation, and executive function, ADHD is worth considering — especially if you have a history of these difficulties that felt more manageable when you were younger.Perimenopause is a time of significant estrogen fluctuation and decline. Since estrogen affects dopamine systems, this can make ADHD symptoms worse.
Yes.
Women with ADHD appear to have higher rates of PMDD than the general population. Both ADHD and PMDD involve dopamine and serotonin systems, and both can involve emotional dysregulation.
If you have severe premenstrual symptoms and ADHD, ask your provider specifically about PMDD..
In the week or two before menstruation, estrogen drops.
Because estrogen supports dopamine activity, this drop can reduce dopamine support in the brain. ADHD brains are already more vulnerable in this system.
The result may be:
worse focus
more emotional reactivity
reduced working memory
lower frustration tolerance
more fatigue
less effective ADHD medication
Tracking this pattern can help you plan around it.
Yes.
Women with ADHD have higher rates of postpartum depression and postpartum anxiety.
The sharp postpartum drop in estrogen and progesterone can affect dopamine systems. Sleep deprivation makes this harder. ADHD can also make the demands of postpartum life harder to manage without support.
If you have ADHD and are pregnant or postpartum, proactive planning with your care team is important.
The Bigger Picture
For too long, the hormonal dimension of ADHD in women has been missed.
Women were told their symptoms were PMS, stress, anxiety, motherhood, or normal aging. The ADHD piece was missed. The hormone piece was missed. The interaction between the two was missed.
That left many women trying to manage real changes in brain function without language, treatment, or support.
This is changing, slowly.
More research is being done. More providers are learning about ADHD in women. More women are recognizing the pattern and bringing better questions to their care teams.
You deserve care that accounts for your ADHD, your hormonal biology, and the way the two interact across your lifespan.
Continue Exploring
- ADHD in Women — the complete picture
- ADHD and PMDD
- ADHD and HRT
- Dopamine and ADHD
- ADHD and Sleep
- ADHD and Anxiety
- ADHD Burnout in Women
- ADHD Sensory Overload
- ADHD and Eating Disorders
- ADHD and the Menstrual Cycle
- ADHD and Menopause
- ADHD and Pregnancy
- ADHD and Migraines in Women
If you are a woman with ADHD navigating the hormonal dimension of your symptoms, I offer neurodivergent-affirming therapy and support via telehealth in North Carolina and South Carolina. I bring 31 years of clinical experience and a deep understanding of how ADHD actually shows up in women's lives — including the parts that most providers miss.
Work with Kristen McClure | Learn more about neurodivergent-affirming support
