
ADHD Burnout in Women
There is a kind of exhaustion that goes beyond being tired.
You may still be going to work answering messages, keeping appointments, and handling the basic logistics of your life. From the outside, things may look fine.
Inside things might not feel fine.
You may feel foggy where you used to feel clear. You may feel irritable in ways that surprise you. You may stop caring about things that used to matter. Not because you chose to stop caring, but because you have very little left.
If you are an ADHD woman, this is not a personal failure. It is a sign that the load has been too high for too long.
ADHD burnout can happen when a nervous system that already works hard has been pushed past what it can keep doing. For many ADHD women, burnout builds after years of masking, overperforming, and compensating.
These strategies may help you get through the day. They are not meant to be a permanent way to live.
Understanding what ADHD burnout is, and what recovery requires, is where the work begins.
What ADHD Burnout Is and Is Not
ADHD burnout is a state of deep exhaustion and reduced functioning.
It often includes:
- cognitive fatigue
- sensory overload
- emotional strain
- lower tolerance for demands
- loss of capacity that feels different from your usual self
ADHD burnout is not laziness or proof that you are getting worse at managing ADHD.
It is also not the same as depression, although ADHD burnout and depression can look similar and can happen at the same time.
Burnout happens when the demands on your nervous system are greater than what your nervous system can keep doing.
The ADHD brain often uses more effort than people realize for ordinary tasks. Regulating attention, switching tasks, filtering sensory input, holding information in working memory, and managing impulses can all take active effort.
Much of that effort is invisible.
When years of ADHD masking are added on top of that, the cost increases. You may be performing competence, hiding struggles, compensating for gaps, and trying to look fine while using more energy than anyone sees.
Burnout is when that cost catches up with you.
ADHD burnout has not been studied as much as occupational burnout or autistic burnout.
But ADHD women describe this pattern often, and clinicians see it. The research may still be developing, but the lived experience is real. In many ways it is similar to autistic burnout.
Why ADHD Women Are Especially Vulnerable to Burnout
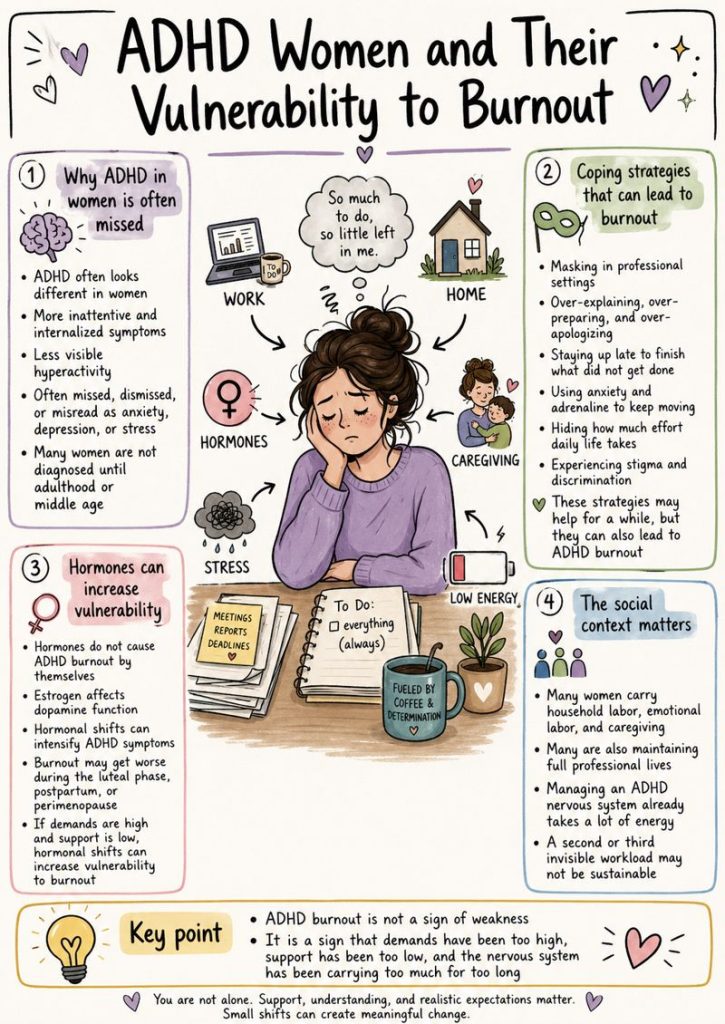
ADHD often looks different in women.
Many ADHD women have more inattentive and internalized symptoms. They may not show the more visible hyperactivity that tends to get noticed earlier.
Because of this, ADHD in women is often missed, dismissed, or misread as anxiety, depression, or stress.
Many women reach adulthood, or even middle age, without knowing that ADHD is part of what they have been managing.
Without that knowledge, and without useful accommodations, ADHD women often build coping strategies that help them get by but do not protect them over time.
They may:
mask in professional settings
over-explain, over-prepare, and over-apologize
stay up late to finish what did not get done
use anxiety and adrenaline to keep moving
hide how much effort daily life takes
experiencing stigma and discrimination
These strategies can work for a while. They can also become part of the path into burnout.
Hormonal changes can add to the risk of ADHD burnout.
Estrogen directly affects dopamine function, which means the hormonal shifts of the menstrual cycle, perimenopause, and postpartum periods can intensify ADHD symptoms. Many women notice that what feels like ADHD burnout often escalates during the luteal phase of their cycle, or accelerates during perimenopause, when estrogen levels drop and previously useful coping strategies stop working. If demands were high and support was low, different phases of a womens cycle or life increases vulnerability.
The social context matters too. Women are still more likely to be responsible for household labor, emotional labor, and caregiving, often while maintaining full professional lives. When an ADHD woman is already spending enormous energy managing her own nervous system, adding a second or third invisible workload may not be sustainable.
ADHD burnout is not a sign that you are weak. It is a sign that you were doing too much, without enough support, for too long.
Signs of ADHD Burnout

ADHD burnout does not always look like collapse from the outside. Many women continue working, caregiving, and meeting obligations while they are in full burnout. The functioning may look intact. The internal experience is different.
Cognitive signs of ADHD burnout
Cognitively, burnout often looks like fog. Words that used to come easily do not come. Tasks that were routine now require enormous effort to start. Memory gaps widen. Decisions that should be simple feel paralyzing.
Emotional signs of ADHD burnout
Emotionally, ADHD burnout can look like flatness and irritability.
You may feel numb or disconnected. You may feel irritated by things that would not usually bother you. This can be part of emotional dysregulation in ADHD.
Things that used to feel good, or that you used to enjoy, may not feel good right now.
Your emotional range may feel smaller. Your tolerance for everyday demands may shrink.
Sensory signs of ADHD burnout
Sensorially, the world can feel louder.
Fabrics, sounds, light, crowded spaces, and everyday noise may become harder to filter. Sensory overload that was already hard to manage can become almost impossible to push through.
Overstimulation that you could handle before may now trigger a response that feels hard to control.
Social Signs of ADHD Burnout
Socially, connection that used to feel supportive can start to feel like a demand.
Even people you love may feel like too much. The social mask, which already took energy to maintain, may fall away. Or you may keep holding it up, but at a cost that leaves little energy for anything else.
This is one reason ADHD burnout can be hard to recognize in women. From the outside, the symptoms may look like depression, stress, lack of effort, or withdrawal.
The problem is that ADHD burnout may be invisible to others. Many women keep working, caregiving, answering messages, and meeting obligations while they are burned out. Because they are still functioning, other people may not see how much capacity has been lost.
This makes burnout hard to name. It also makes it easy to keep pushing until the burnout becomes a crisis.
ADHD Burnout vs. Depression: Key Differences
ADHD burnout and depression can look similar from the outside.
Both can involve exhaustion, low motivation, difficulty starting tasks, irritability, emotional flatness, sleep changes, and trouble concentrating.
The difference is often in what is driving the shutdown.
Depression is a mood disorder. The main problem is a persistent change in mood, pleasure, hope, and interest. A person may feel low, empty, worthless, hopeless, or unable to enjoy things even when demands are reduced.
ADHD burnout is usually a depletion state. The main problem is that the person has been coping with too much demand for too long. The nervous system is overloaded. Daily life has required more executive functioning, masking, sensory tolerance, emotional regulation, and recovery than the person had available.
This difference matters because the first step may be different.
For depression, treatment often includes therapy, medication, or both. One common treatment approach is behavioral activation, which helps a person gradually re-engage with meaningful activity, routine, social contact, and sources of pleasure or mastery.
For ADHD burnout, the first step is usually not adding more activity. It is reducing demand and increasing support. This may include fewer obligations, more rest, sensory relief, practical help, lowered expectations, workplace or school accommodations, simpler routines, and more recovery time.
A simple way to think about the difference:
| Question | More like ADHD burnout | More like depression |
|---|---|---|
| What is the main issue? | Depletion from prolonged demand | Persistent low mood, hopelessness, or loss of pleasure |
| What often helps first? | Fewer demands, more support, more recovery | Treatment that may include therapy, medication, and gradual re-engagement |
| What happens when demands decrease? | Symptoms may start to ease | Symptoms may continue even when life is quieter |
| What happens if more activity is added too soon? | It may worsen depletion | It may help if done gradually and with support |
| What is the clinical risk? | Burnout can be missed if it is treated only as low motivation | Depression can be missed if everything is explained as burnout |
In real life, ADHD burnout and depression can also overlap.
ADHD burnout can trigger or worsen depression. Depression can make ADHD symptoms harder to manage and can make burnout happen faster. A good clinical picture looks at both.
One useful question is:
Does the flatness and exhaustion feel mainly connected to the demands, masking, sensory load, and constant effort of daily life? Or does it stay present even when those demands are lower?
If there are thoughts of self-harm, feeling unsafe, persistent hopelessness, or a sense that life is not worth living, that needs immediate support from a clinician, crisis line, or emergency service.
ADHD women in burnout often have a loud inner critic. That critic may interpret burnout as failure.
It may feed the shame that has built up over years of struggling without an accurate explanation.
That narrative interferes with recovery.
You cannot recover well while telling yourself that needing rest means you have failed.
Time matters. ADHD burnout does not resolve in a few days.
Depending on how long it has been building, and how depleted your nervous system is, recovery often takes weeks to months. Trying to rush recovery often makes it take longer.
How the Empowerment Model Supports ADHD Burnout Recovery
My work with ADHD women is organized around five areas. In ADHD burnout recovery, each one has a specific role.
Self-Awareness
Self-Awareness is the starting point.
Before you can recover from ADHD burnout, you need to understand how you got there. This means looking at which demands exceeded your capacity, what your early warning signs were, and what your burnout looks like for you.
Self-awareness is not about blame. It is about building a map, so you are not trying to recover without information.
Self-Compassion
Self-Compassion is not optional in ADHD burnout recovery.
Shame often builds around burnout:
- I should be able to handle this.
- Other people manage more than I do.
- What is wrong with me?
These thoughts are not a minor problem. They can directly interfere with the rest and recovery your nervous system needs.
Working with the shame, instead of pushing past it, is part of the work.
Self-Accommodation
Self-Accommodation is where the practical changes happen.
This means identifying what your nervous system actually needs to function. Not what you think you should be able to manage.
Then you build your environment and routines around that reality.
For women in ADHD burnout, self-accommodation often means reducing demands before rebuilding. It means asking what you can stop doing before asking what you should do differently.
Self-Advocacy
Self-Advocacy becomes important as you recover and as you begin to prevent future ADHD burnout.
It means developing language for your needs with partners, employers, healthcare providers, and yourself.
It also means learning to believe those needs are legitimate.
Many ADHD women have a long history of having their needs treated as inconveniences. Rebuilding the confidence to advocate for what you need can take time.
Self-Care
Self-Care in ADHD burnout is not about adding more wellness practices to an already overwhelmed system.
It is about the basic conditions your nervous system needs to recover:
- sleep
- adequate nutrition
- some movement
- genuine rest
Genuine rest is different from scrolling through your phone because your brain cannot stop.
These are not luxuries. For an ADHD brain in burnout, they are prerequisites.
Frequently Asked Questions
ADHD burnout is a state of deep exhaustion and reduced functioning that happens when an ADHD nervous system has been operating above its capacity for too long. It often includes cognitive fog, emotional flatness or irritability, sensory sensitivity, and a loss of coping capacity. It is different from ordinary tiredness. Recovery usually requires structural changes, not rest alone.
Occupational burnout is driven primarily by workplace demands. ADHD burnout is broader and often deeper. It reflects the cumulative cost of managing an ADHD nervous system in a world not designed for it — years of masking, compensating, and overperforming that extend far beyond any single job or relationship. Many ADHD women experience burnout even in jobs they find meaningful, because the depletion is not about the work itself but about the ongoing effort of being an ADHD person in a neurotypical environment.
The key difference is that ADHD burnout is connected to context. It happens when demands exceed capacity, and it often improves when those demands are reduced and support is added. Depression is a mood disorder that can happen even when circumstances change, and it usually needs its own treatment. The two can occur together, and ADHD burnout can contribute to depression. If reducing demands and adding support does not lead to any improvement over time, depression may be part of the picture, and it is worth working with a clinician who can assess both.
This depends on how long ADHD burnout has been building, how depleted your nervous system is, and how much your conditions actually change. Mild burnout with real support may begin to lift in weeks. Severe or long-standing burnout, especially without structural change, can last for months. There is no reliable timeline. Trying to rush recovery or return to full demands too quickly often makes ADHD burnout last longer. Recovery is usually uneven, with better days and worse days, before it becomes more stable.
Recovery from ADHD burnout usually requires three things: a real reduction in demands, a real increase in support, and accommodations that allow your nervous system to work within its actual capacity. It also means addressing the shame and self-criticism that often come with burnout, because those can interfere with the rest your system needs. Therapy can help here, not by adding more to do, but by helping you work through the internal barriers to recovery and identify realistic structural changes. A medication review, hormonal evaluation if relevant, and an honest look at what you are carrying may also be worth considering.
You Were Not Built to Burn Out Quietly
Many women with ADHD have spent years pushing past their limits to be accepted, understood, or seen as capable. Over time, that can cause ADHD burnout.
If you are in North Carolina or South Carolina and think therapy might support your recovery, I would be glad to hear from you.
Continue Exploring
Ready to work with someone who understands ADHD burnout in women?
I offer neurodivergent-affirming telehealth therapy for women in North Carolina and South Carolina. My work is organized around the Empowerment Model — not symptom management, but building a life that fits how your brain actually works.
Email: kristenlynnmcclure@gmail.com
$110/session | 55 minutes | Most BCBS plans accepted | Telehealth only | Licensed in NC and SC
