ADHD and Alcohol in Women: Understanding the Self-Medication Pattern
By Kristen McClure, MSW, LCSW | Neurodivergent-affirming therapy for women

At the end of a hard day, alcohol may feel like relief.
You may have been managing too much, holding too many things in your head, and trying to appear composed when you did not feel composed. Then you have a drink, and for a little while, the mental noise gets quieter. Self-criticism softens. Your body gets a break from managing.
That relief is real. It is not weakness or a character flaw. For ADHD women, alcohol can offer temporary relief from a nervous system that has been working hard all day. It may create a short-term sense of calm, quiet, or lowered pressure that is harder to access without support.
Understanding why ADHD and alcohol can become connected is the beginning of a more honest relationship with both.
The Neuroscience Behind ADHD and Alcohol
ADHD involves dysregulation in the dopamine and norepinephrine systems. These brain chemicals help regulate motivation, reward, alertness, focus, emotional regulation, and impulse control.
Many ADHD brains operate with lower baseline arousal, which means the brain may seek more stimulation to feel alert and engaged. This can make it harder to start tasks, sustain focus, regulate emotions, and manage impulses.
Alcohol can create a rapid chemical shift in the brain. It can increase dopamine release, lower activity in the prefrontal cortex, and activate GABA systems that slow the nervous system. The prefrontal cortex is involved in self-monitoring, impulse control, and self-criticism. GABA helps quiet nervous system activity.
For ADHD brains, this can feel like temporary relief. Many ADHD people live with a difficult mix of sensory and emotional overload, while also struggling to generate enough activation for attention, focus, and task initiation. Alcohol may briefly create a sense of calm, quiet, or lowered mental pressure.
In the short term, alcohol may seem to work. The problem is that the brain adapts. Over time, the same amount of alcohol may have less effect, tolerance can build, and the brain’s chemical baseline can shift in ways that make ADHD symptoms harder to manage.
The morning after drinking may bring more anxiety, weaker executive function, poorer focus, and stronger emotional dysregulation. For some ADHD people, this creates a cycle: alcohol brings short-term relief, but the aftereffects make the next day harder. That harder day can increase the urge to drink again.
Why Women with ADHD Are at Particular Risk
Research consistently shows that ADHD people have higher rates of alcohol and substance use disorders than the general population. For ADHD women, several factors may increase vulnerability:
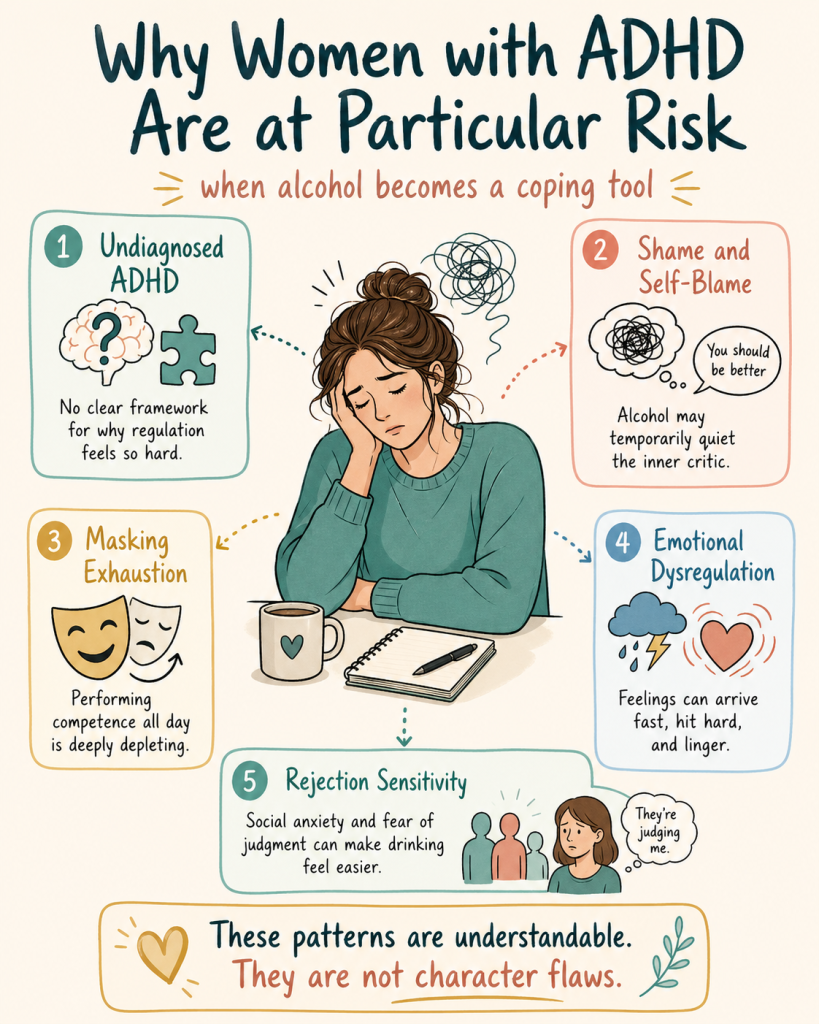
Many ADHD women do not know they have ADHD. Without that framework, it can be hard to understand why regulation feels so difficult.
Alcohol may seem to help because it briefly turns down the volume. Without ADHD context, that pattern may look like coping rather than a warning sign.
ADHD women often carry shame about struggles with forgetting, inconsistency, emotional intensity, and follow-through. Alcohol can temporarily quiet that internal criticism.
That shame often comes from years of unrecognized and unsupported ADHD.
Performing neurotypical competence all day is depleting. Alcohol can feel like an exit from that performance.
For ADHD women who mask heavily, drinking may become a way to stop managing, monitoring, and holding everything together.
ADHD emotional intensity can make feelings arrive quickly, feel strong, and linger longer. Without effective regulation tools, alcohol may become a way to blunt that intensity for a short time.
Social anxiety, fear of judgment, and sensitivity to rejection are common in ADHD. Alcohol can reduce social anxiety in the short term and make social situations feel easier to manage.
Recognizing the Pattern Without Shame
For ADHD women, using alcohol to self-medicate is often a response to a real regulation problem. It is not a character flaw. It may mean your nervous system has been under-resourced and alcohol has become a quick way to manage distress, overload, or exhaustion.
That does not make alcohol a safe long-term strategy. But understanding the function it serves makes it easier to find safer supports.
Questions to Ask Yourself
- Does alcohol feel different for me than it seems to for other people?
- Do I look forward to drinking as relief, not just pleasure?
- Do I drink more than I planned?
- Is drinking connected to overwhelm, shame, social exhaustion, or rejection sensitivity?
- Has drinking become harder to control as my stress has increased?
These questions are not about blame. They help clarify what your nervous system is trying to manage.
ADHD Treatment and Alcohol
Research shows that effective ADHD treatment can reduce the risk of substance use problems. When ADHD is better supported through medication, therapy, accommodations, and daily structure, alcohol may become less necessary as a regulation tool.
Many ADHD women notice that their relationship with alcohol changes after ADHD treatment begins. This is not because ADHD medication treats alcohol use directly. It is because the medication and adhd support may reduce the underarousal, emotional dysregulation, and cognitive overwhelm that alcohol was temporarily managing.
Treating alcohol use without recognizing ADHD can miss the underlying pattern.
How the Empowerment Model Supports ADHD Women With Alcohol Concerns
Self-Awareness
Start by understanding what alcohol does for you.
- Does it reduce emotional intensity?
- Quiet self-criticism?
- Lower sensory overload?
- Help with social anxiety?
The specific function matters because it points toward what needs support.
Self-Compassion
Shame can keep the alcohol cycle going. Many ADHD women blame themselves for needing relief, especially after years of being unsupported.
Self-compassion does not mean ignoring alcohol concerns. It means reducing the shame that makes the pattern harder to interrupt.
Self-Accommodation
Alcohol may be substituting for regulation tools that were never taught or supported. Helpful accommodations may include body-based regulation, better sleep support, structured wind-down routines, sensory breaks, and lower evening demands.
The focus is reducing the load alcohol has been helping you carry.
Self-Advocacy
Support is more effective when providers understand the ADHD-alcohol connection. Generic addiction treatment may miss the role of executive dysfunction, sensory overload, emotional intensity, masking, and shame.
Being able to say, “Alcohol has been one way my nervous system manages overload,” can help you get more accurate care.
Self-Care
Sleep, nutrition, movement, sensory regulation, and recovery time are not minor supports. They are part of the infrastructure ADHD nervous systems need to regulate.
When basic needs are neglected, alcohol can become more appealing because the nervous system is already strained.
Frequently Asked Questions
ADHD women can have differences in dopamine and norepinephrine systems that make emotional regulation, sensory filtering, and cognitive control more effortful. Alcohol can temporarily reduce that strain by increasing dopamine release and slowing nervous system activity. When ADHD is undiagnosed, chronic masking, exhaustion, and shame can make alcohol feel like an understandable form of self-medication.
Not exactly. Alcohol is a central nervous system depressant, but for ADHD brains it may temporarily quiet mental noise, reduce self-monitoring, and soften the internal critic. It can also create a short-term dopamine shift that feels like relief from ADHD-related tension. The effect may feel calming, but alcohol does not address the underlying ADHD-related regulation challenges and can worsen focus, mood, sleep, and executive function over time.
Research suggests that effective ADHD treatment may reduce substance use risk. When ADHD medication, therapy, accommodations, and regulation skills address the underlying ADHD-related dysregulation, alcohol may become less necessary as a coping tool. This is one reason ADHD and alcohol concerns should be understood together, rather than treating alcohol use in isolation.
Key signs include drinking for relief rather than pleasure, drinking after ADHD-related stress, drinking more than intended, and noticing that alcohol has become more important over time. If drinking is tied to overwhelm, social exhaustion, emotional flooding, or shame, it may be serving a regulation function that is worth looking at honestly.
Sometimes, indirectly. If ADHD medication helps reduce overwhelm, support emotional regulation, and quiet internal pressure, the pull toward alcohol may lessen. This is not guaranteed, and women with alcohol dependence usually need additional support. ADHD and alcohol concerns are often best addressed together.
If alcohol has become a regular part of how you get through the day, that does not mean you have a character flaw. It may mean your nervous system has been under-supported and found something that worked temporarily, but with a cost.
Understanding what alcohol has been helping you manage can point you toward support that meets those needs more safely.
Continue Exploring
- ADHD in Women — the complete picture
- ADHD and Emotional Dysregulation
- ADHD and Shame
- ADHD Masking in Women
- Rejection Sensitive Dysphoria
- ADHD Burnout in Women
- ADHD and Sleep
- ADHD and Cortisol in Women
- Late ADHD Diagnosis in Women
I offer neurodivergent-affirming therapy for women with ADHD across North Carolina and South Carolina via telehealth. If you recognize your nervous system in this page, I'd be glad to talk. Learn more about working with me.
